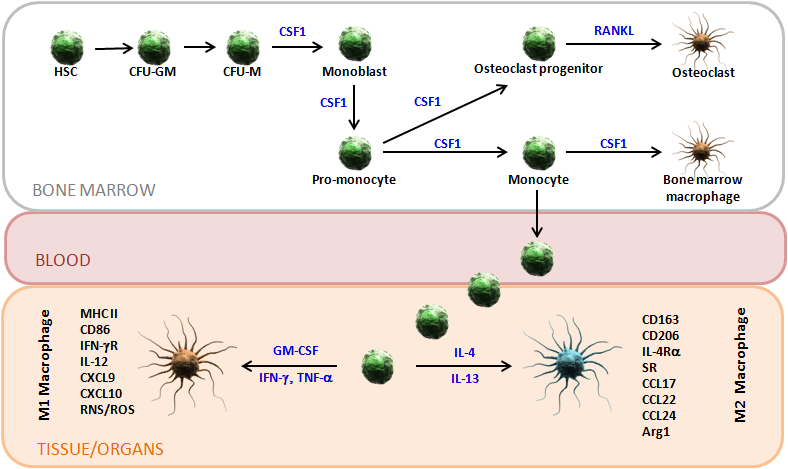
Macrophages are very important members of the mononuclear phagocytic system. This notoriously heterogeneous system is composed of macrophages themselves in addition to dendritic cells, monocytes and their lineage committed progenitors. Although there is a lot of overlap between these cells types, regarding both cell surface markers and function, there are still some distinct features that can uniquely identify them.
Nowadays, it is almost impossible to talk about macrophages without mentioning dendritic cells, and vice versa. However, the most important and most widely accepted difference between these two types of cells is their capacity to stimulate naïve T cells. When it comes to their antigen presentation capacity, dendritic cells are superior. However, macrophages are heavily involved in a number of other metabolic functions, such as pathogen killing and wound and tissue repair, where dendritic cells are less prominent.
 Login / Register
Login / Register 








Follow Us